Restrictive interventions are those which restrict an individual’s freedom to move or behave. They include, but are not limited to, mechanical restraints, manual holds, seclusion, psychotropic medication or intensive staffing to control the occurrence of certain behaviors. (See this link for an example of a policy on the use of restrictive interventions) 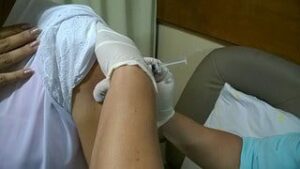
The ultimate result when one uses some form of restrictive intervention is that a target behavior is interrupted and stops. At times, when a behavior escalates to the point that there is danger to self or others, there is a justification for the use of restrictive interventions. However, the ease with which behaviors can be interrupted by such interventions, leaves room for them to be used (and sometimes abused) in place of other less restrictive interventions that may require more effort from staff.
 It is important to note that every behavior serves a function, and all behavior is interconnected in a behavior web—that is, the behavior of one person is affected by the behavior of another and vice versa. When a patient or student engages in challenging behavior, it is essential that we understand what is the function of the behavior and what are the variables maintaining it. Once these elements are identified, it is easy to design less restrictive interventions that will leave to the acquisition of alternative replacement behaviors that serve the same function.
It is important to note that every behavior serves a function, and all behavior is interconnected in a behavior web—that is, the behavior of one person is affected by the behavior of another and vice versa. When a patient or student engages in challenging behavior, it is essential that we understand what is the function of the behavior and what are the variables maintaining it. Once these elements are identified, it is easy to design less restrictive interventions that will leave to the acquisition of alternative replacement behaviors that serve the same function.
In designing interventions that will serve to teach skills that can replace challenging behavior, it is essential to take into consideration what recommendations the staff will be able to follow. You may design the best, scientifically sound intervention, and if your staff is not prepared to support that intervention it will fail. Remember, for the staff, restrictive interventions have a fast payoff—the behavior of concern stops fast. You will need to create an intervention that will 1) not require too much effort and 2) will lead to a sharp decrease in the frequency or intensity of the problem behavior.
Let me tell you about a patient I once had and what intervention we used to reduce the need for restrictive intervention:
 Ms. “A” was a woman over 50 years old, with a history of schizophrenia, who had been taking psychotropic for many years and had developed tardive dyskinesia, with a protruding tongue, for whom spoken speech was very difficult. She had frequent (at least once a day) “codes”, where she broke property, and sometimes could become physically aggressive. As the result of the codes, she would receive intramuscular medication, and sometimes, it could lead to mechanical restraints or increased observation levels with a constant 1:1 staff monitoring her all day.
Ms. “A” was a woman over 50 years old, with a history of schizophrenia, who had been taking psychotropic for many years and had developed tardive dyskinesia, with a protruding tongue, for whom spoken speech was very difficult. She had frequent (at least once a day) “codes”, where she broke property, and sometimes could become physically aggressive. As the result of the codes, she would receive intramuscular medication, and sometimes, it could lead to mechanical restraints or increased observation levels with a constant 1:1 staff monitoring her all day.
In order to design the intervention for this woman, I observed her and her interactions with people around her. I noticed that since she could not speak, people would not talk to her either. At one point, I watched her stand by the nurses’ station for two hours, while people walked by without even looking at her. After those two hours, she quietly walked to the exit door and pulled the swipe mechanism off the wall. Naturally, a code was called and over ten people were now addressing her. A psychiatrist and an internist needed to perform assessments, a nurse needed to monitor how she responded to the intra-muscular medication, and a staff was assigned to monitor her behavior, to make sure she would not destroy any more hospital property. As you can see, her behavior had a clear payoff: attention and interaction with staff members.
The intervention for her was simple and easy to follow: as you walk by her make sure to give her eye contact, and at least a nod of the head. If you have some time, give her some extra attention by using simple statements or yes/no questions (e.g. Hi Ms. A, it’s a beautiful day, right?) that she could reply with a simple nod or head shake. The data indicated that she could tolerate up to two hours without the direct interaction, so even if only a small percentage of the staff followed the recommendations, it would be likely that someone would acknowledge her presence and interact with her at intervals shorter than two hours. Problem solved. No more codes until discharge.
Using behavior science allowed me to understand the function of this patient’s behavior, the variables that were maintaining it, and how this behavior affected the behavior of staff. Behavior analysis is a viable alternative to restrictive interventions. It is evidence-based, person-centered and cost effective. It is time that more behavior analysts get involved in the care of behavioral health patients.
What do you think? Comment below, and let me know what kind of problems you face in your setting that lead to restrictive intervention. How do you and your organization respond to it? What measures have you and your organization taken to reduce the use of restrictive interventions?


While working for group homes I was responsible for developing behavior intervention plans. The plans were reviewed by new staff under the supervision of a behavior specialist and monthly review of plans for all staff members were required. One thing that I found helpful in preventing restrictive interventions from being used unnecessarily was the emphases of using restrictive interventions as a last resort. In our plans a statement was written that staff is required to use the least restrictive interventions (proactive strategies, active strategies and teaching components for replacement behaviors,etc.), before using more restrictive interventions. The agency was also responsible for investigating incidents in which restrictive interventions were used and to ensure that the right to use the interventions in these circumstances were not abused by staff. Overall, preventive measures as well as accountability for such measures were encouraged to protect our individuals.
You’re right. Proactive measures are always better.